
Created with the collaboration of Dr. Marchetti, D.: freelancer in Statistics
INTRODUCTION
Obesity was a rare situation before the twentieth century, but now obesity and pandemic have become almost synonymous, and Italian data reflect this sad forecast of epidemiological data. In Italy 35% of the population is overweight and 10% obese [3]. The World Health Organization (WHO) has officially recognized obesity as a global epidemic. [1]
In 2005, the WHO estimated that at least 400 million adults (9.8%) were obese, with higher rates among women than men [2]. According to the seventh report of the Institute Auxologico of Milan (Italy) on the obesity issue, announced last year, for those between the age of 45 and 64, only one out of three men has a normal weight, while, for women, the ratio is one to one. 36% of children, by the age of eight (the peak age), are overweight or obese. Obesity is increasing of 2.5% every 5 years [3].
OBJECTIVE
The purpose is to evaluate a practical and fast way to weight loss and health improvement that uses only the biochemical properties of food, without giving any indications on the amount, in other words on calories. The method used is the Bioimis Nutritional Program.
METHODS AND MATERIALS
The studied sample is composed of individuals averagely aged 43.8 years, age range from 18 to 82 years (with a minimum of 18 and a maximum of 82). Males are on average older (45.1 years), females are younger (43.3 years).
The average height is 1.65 meters, with a minimum of 1.20 and a maximum of 1.92.
The sample studied has followed a nutrition without limits in the quantity of food and extra virgin olive oil as specified by the Bioimis Nutritional Program. Each person received a menu made of breakfast, lunch and dinner to follow for 2 consecutive days, the second day the person would have called and been provided with the next menu for the following 2 days.
For the following analysis all customers were considered, regardless of the number of months they took part in Ideal Fit Plan.
The table below shows the frequencies of customers for the number of months of Ideal Fit:
Within the sample used for analysis, there are individuals with certain medical conditions such as diabetes, hypertension and thyroid disease.
Specifically, about 7% of the sample is diabetic, 3% have impaired thyroid function and 22% is hypertensive.
RESULTS
Considering the type of variables to be analyzed (quantitative), and having as objective the comparison of some values in two different times (at the beginning and end of treatment), the best suitable statistical tool for this type of analysis is the t test with paired data [1]. This test compares the average score of the two groups, and allows to understand if the difference between the two averages is due to chance (linked to the current sample) or it is statistically significant (meaning it is real, of important relevance and extensible to the entire population).
Before applying the t test, it is necessary to evaluate the equality of the two group variances in question (in this case the group of subjects is unique, and taken at two different times). The performance of this assessment is carried out by the test statistic relationship between the variances [2]. Therefore, before each t test the test on the variances will be reported (which will not be commented because of no conceptual relevance for this study, being it only instrumental).
For each variable of interest, find below a summary table with the minimum, maximum, and average value used (differing for each variable because of the presence).
Weight
The average initial weight is 91 kg, with a minimum value of 41kg and a maximum value of 217Kg. After treatment, the values tend to be lower: the average weight of 7kg decreases and becomes equal to 84Kg, the minimum value becomes 44Kg, and the maximum is 186Kg.
From the average values obtained, by dividing the sample into two groups based on gender, males seem to have a greater weight decrease due to the treatment (average value 9 kg difference) than women (7kg difference).
By analyzing the equality of averages, it will be shown if these differences are related to the randomness of the sample used, or if they can relate to the whole population.
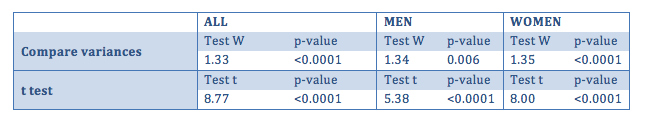
Both for the general sample and gender-divided samples it was necessary to use the t test for groups with different variance. In fact, "after treatment" the group demonstrates to have a different variance from the "before treatment" group. This means that the two groups ("before" and "after") have a different variability (both in the general case sample and in males and females).
The t test is significant in all comparisons, this means that the "before" average weight are significantly different from the "after" treatment averages, with a p-value less than 0.0001.
In addition to the tests reported in the chart, t one-sided test was used to help understand the direction of the inequality (meaning, which of the two averages is greater). Regarding the weight, the one-sided test shows a p-value less than 0.0001 in favour of weight loss: the "after" weight is on average less than the "before" weight, both in the general sample and in the male and female samples.
On average, weight loss for the overall sample is 10.7kg, the customer with the most weight loss registers a weight of 39kg, while the customer with the lowest result gained 2kg.
For the female group, the average weight loss is 9.9kg, with a maximum loss of 24.0Kg (the minimum loss was -2kg, i.e. an increase in weight).
For the male group, the average weight loss is 13.3 kg, with a minimum loss of -1.1 kg and a maximum loss of 39.4 kg.
An Analysis of variance (ANOVA), between the two genders, was performed to study the weight loss occurred during the Ideal Fit month.
The result agrees with what stated in the previous steps: the two groups are significantly different (F = 111.16 test with p.value <0.001). This means that the customer's gender affects the amount of Kg they manage to lose.
BMI
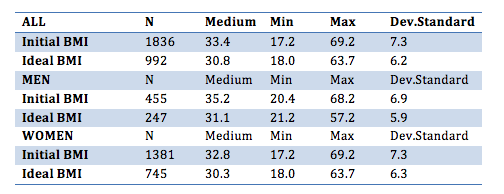
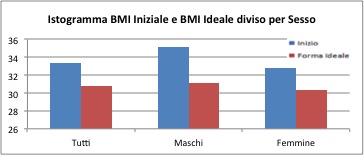
The average initial BMI is equal to 33 for the general sample, 35.2 for males, and 32.8 for females. The standard value at the end of the treatment is of 30.8 for the total sample, 31.1 for males, and 30.3 for females.
The group of females reported greater variability, with a minimum value ranging from 17 for the initial BMI and 18.0 for the ideal BMI, up to a maximum values of 69.2 for the initial BMI and 63.7 for the ideal BMI.
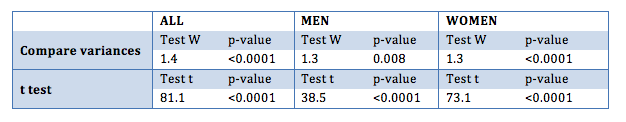
The results of the t test for BMI are similar to the results obtained for the average weight (BMI is in fact a transformation of weight): t test is significant for all the samples, meaning that the initial BMI is significantly different from the ideal one.
Specifically, the one-sided test, the initial BMI is greater (p-value less than 0.0001) than the ideal.
In general, the average difference is 3.9 points, with a minimum value of -0.9 and a maximum of 11.5.
For the group of males, the standard average difference of the "before" - "after"score, is 4.3 points (with a minimum of -0.3 and a maximum of 11).
For the group of females, the average difference is 3.8, with a minimum value of -0.9 and a maximum of 8.9.
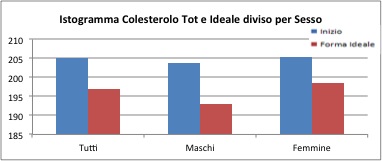
Cholesterol
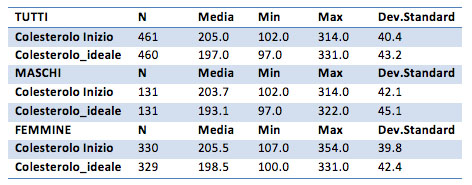
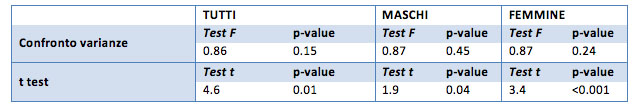
Considering the one-sided hypothesis we understand that, specifically, the ideal cholesterol is on average lower than the initial cholesterol (p-value of <0.01).
Considering only the group of males, the difference remains evident: total cholesterol is different from the ideal initial cholesterol, in particular is greater than the initial one (alternative hypotheses with p-value <0.001).
For the female group the difference between the initial and ideal cholesterol is very obvious (p-value equal to 0.001). This case also shows that the ideal cholesterol is lower (p-value equal to one-sided hypothesis 0.0003) compared to the initial cholesterol.
On average cholesterol decreases of 8 mg / dl, with a maximum loss of 170 mg / dl, and a loss of -134 mg / dl ( an increase).
For the male group, the difference is as much as 10 mg / dl (minimum loss of -134 and a maximum of 170), while for the female group is 6 mg / dl (minimum value of -120 points and a maximum value of 165).
HDL Cholesterol
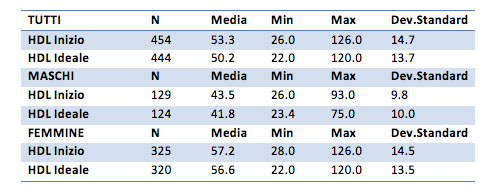

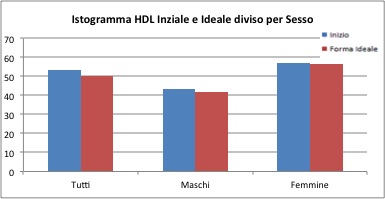
Initial HDL is equal to 53.3 mg / dl for the general sample, 43.5 mg / dl for males and 57.2 mg / dl for females. After treatment, the HDL becomes equal to 50.2 mg / dl for the general sample, 41.8 mg / dl for males, and 56.6 mg / dl for females.
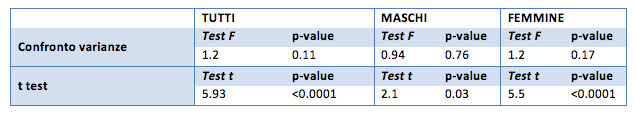
For the overall sample and the female group, the average score of "before" - "after" HDL are statistically very significant, while less significant (p-value equal to 0.03) in the male group.
Considering the one-sided hypothesis, the results show a decrease in HDL score between the time before and the time after treatment (p-value <0.001 for females and overall champion, for males p-value equal to 0.01). Therefore, the after scores are lower than the baseline scores.
LDL
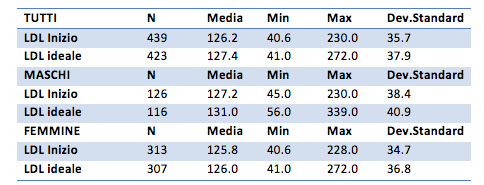
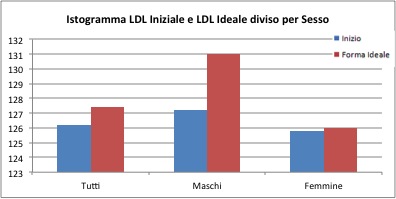
The average values of the initial LDL parameter are 126 mg / dl for the overall sample, 127 mg / dl for males, 125 mg / dl for females. At the end of the treatment they are equal to 127 for the general sample, 131 for males and 126 mg / dl for females. Therefore, it does not seem present substantial differences.
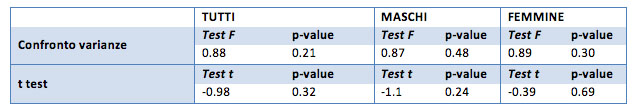
Even the test confirms the equality of the averages in the "before" and "after" treatment sample. Small differences recorded are not significant, and are simply related to the sample "chosen".
Glycated Hemoglobin
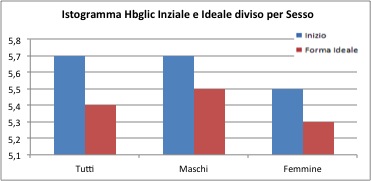
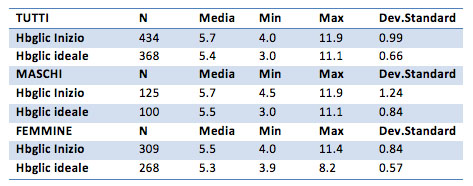 The initial HbA1c scores amount to 5.7% for the overall group, 5.7% for males and 5.5% for females. The final values are equal to 5.4% for the overall group, 5.5% for the male group and 5.3% for the female group. Values themselves do not show much difference, but the t test will verify the inequality.
The initial HbA1c scores amount to 5.7% for the overall group, 5.7% for males and 5.5% for females. The final values are equal to 5.4% for the overall group, 5.5% for the male group and 5.3% for the female group. Values themselves do not show much difference, but the t test will verify the inequality.
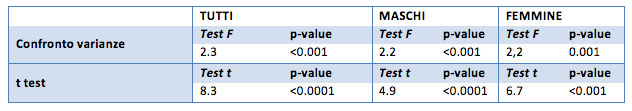 Although the differences are small, the t test confirms a real difference between the "before" group and the "after" group from the treatment (both for the general case, the males group and females group).
Although the differences are small, the t test confirms a real difference between the "before" group and the "after" group from the treatment (both for the general case, the males group and females group).
Specifically, initial Hbglic scores can be considered more at the beginning of treatment (p-value less than 0.001 one-sided hypothesis).
For the general sample, the average loss of Hbglic is 0.36%, with a maximum loss of 5.2% and a minimum loss of -1.9% (an increase).
For the male group the average loss is 0.51% with a minimum of -1.9% and a maximum of 4.8%.
For the female group the average loss during treatment is of 0.30 percentage points, with a maximum loss of 5.2 percentage points and a minimum loss of -1.2 percentage points.
Glycemia
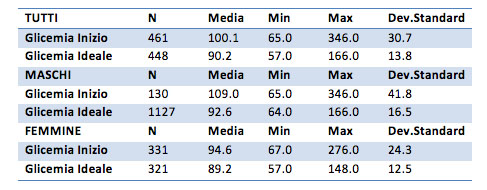
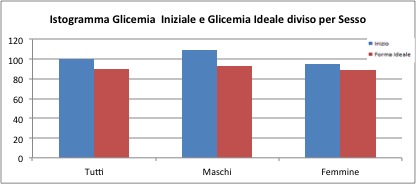
The initial blood sugar value is 100 mg / dl for the overall sample, and after treatment the value drops to about 90 mg / dl. For the group of males only the initial value is 109 mg / dl, and 92.6 mg / dl at the end. For the group of females the initial value is 94.6 mg / dl, and 89 mg / dl at the end. The maximum values recorded for the male group is 346 mg / dl, perhaps "too extreme" and would require a test to check the veracity of this data.
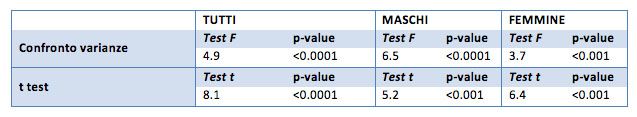
For all three samples considered, there was a significant difference at the level of 0.001 of the "before" and "after" blood glucose values. Considering the one-sided hypothesis there was a significant decrease in blood glucose (p-value 0.001).
For the overall sample, th decrease of blood glucose is 9.9 mg / dL for males only the difference is 16.5 mg / dl, for females only is 7.4 mg / dl.
Triglycerides
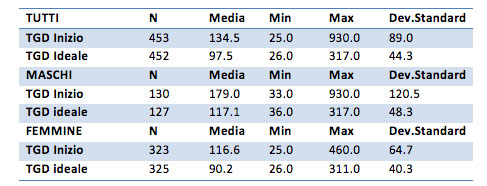
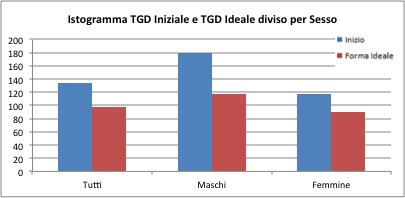
The TGD average for the general sample is equal to 134 mg / dL before treatment and drops to 97 mg / dl after the treatment. For males only, the initial value is 179 points, and at the end of treatment is 117. For females only, the initial average is 116 mg / dl, and at treament concluded is 90.2 mg / dl.
The male group presents a maximum value of 930 points, a very high value for triglycerides. In fact, one of the customers reported this value. We should take into account, for a more detailed analysis, the possibility of eliminating such data due to its uniqueness and uncommonness. However, for the analysis in question it was considered.
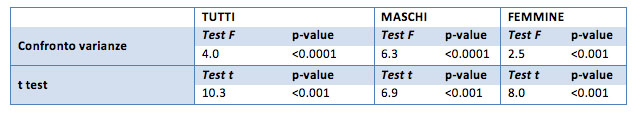
All the samples indicate that the initial average is significantly different from the end of treatment average. Thanks to the one-sided test (p-value <0.0001) the average values recorded at the end of treatment are lower than the initial average values. Specifically, for the overall sample average it is recorded a decrease of 37 points, for males only the decrease amounted 63, for females only amounts to 26 points.
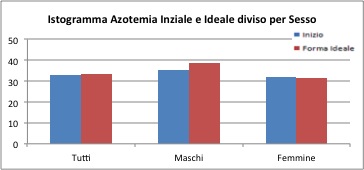
Azotemia
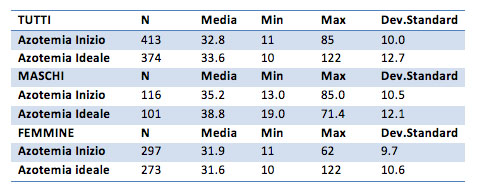
Thanks to the t test, it will be possible to tell if the difference is significant, or can be considered random (that is tied to specific sample).
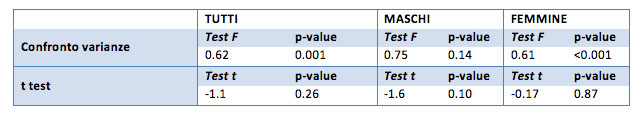
As seen from the p-values reported in the table (all greater than 0.05) the difference between the nitrogen of the "before" and those of "after" does not result significant. Not even the unilateral hypothesis reported significant results.
Therefore, this value does not report a difference between the "before-after" values.
Creatinemia
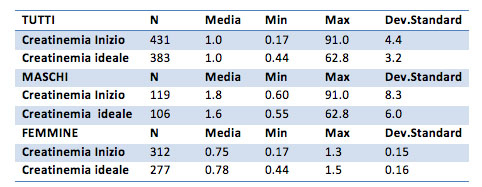
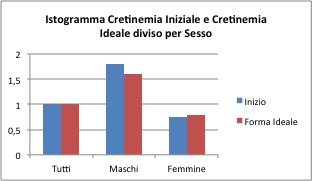
The initial creatinine average values amount to 1.0 mg / dl for the overall sample, 1.8 mg / dl for males and 0.75 mg / dL for females. The average after the treatment is 1.0 mg / dl for the general sample, 1.6 mg / dl for males is 0.78 mg / dl for females.
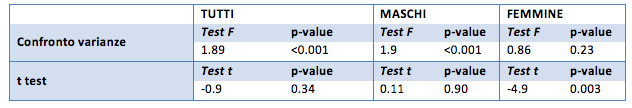
As you could guess from the above table, the sample does not appear to present a general difference between the before and after treatment averages (p-value 0.23). This is found also in the only females sample (p-value 0.26). However, for the group of males there is a significant difference, but this is probably due to the extreme values achieved in this group for both the initial creatinine (91) and the ideal one (62.8). Even in this case is to assess the possibility of not considering these values.
CONCLUSION
In conclusion it can be stated that the treatment produces effects on most of the values considered.
Therefore, to summarize the results we obtain:
- A significant decrease in weight (along with the BMI, being function of the weight itself), total cholesterol, HDL cholesterol, glycated hemoglobin (HbA1c), blood glucose and triglycerides;
- For creatinine, LDL cholesterol and blood urea, there were no significant changes.
ARGUMENT
As mentioned before, the Bioimis Nutritional Program is structured in two Programs. The first program involves an "unconventional" diet that focuses its attention on the biochemical action of foods to maximize weight loss. The intent of this first observation was to check the body's response to this kind of diet to exclude health issues to customers, giving particular attention to renal function, element considered "at risk" in diets with protein content higher than that one indicated by the Mediterranean diet. The results in this regard are considered satisfactory.
Currently, there is an ongoing monitoring of these customers that will provide us with blood tests results performed after three months from the Keep Fit stage and at the end of the first year from the beginning of the program.
BIBLIOGRAPHY
Caballero, «The Global Epidemic of Obesity».;
«WHO | Obesity and overweight».
Italian Istituto Auxologico, «7° Rapporto sull’obesità in Italia - Obesità e genetica: oltre lo stile di vita».
Institute of Medicine of the National Academies: Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein, and amino acids (macronutrients). Wash- ington, DC , National Academies Press; 2002.
Joint Position Statement: nutrition and athletic performance. American College of Sports Medicine, American Dietetic Association, and Dietitians of Canada. Med Sci Sports Exerc 2000, 32(12):2130-2145.
Tarnopolsky M: Protein requirements for endurance athletes. Nutrition 2004, 20(7-8):662-668.
Commentary. International Society of Sports Nutrition position stand: protein and exercise. B Campbell, R B Kreider, T Ziegenfuss, P La Bounty, M Roberts, D Burke, J Landis, H Lopez and J Antonio. Journal of the International Society of Sports Nutrition 2007, 4:8.
Knight EL, Stampfer MJ, Hankinson SE, Spiegelman D, Curhan GC: The impact of protein intake on renal function decline in women with normal renal function or mild renal insuffi- ciency. Ann Intern Med 2003, 138(6):460-467.
Lemon PW: Beyond the zone: protein needs of active individ-uals. J Am Coll Nutr 2000, 19(5 Suppl):513S-521S.
A H. Manninen. High-protein weight loss diets and purported adverse effects: where is the evidence? Sports Nutrition Review Journal. 1(1):45-51, 2004.
Metges CC, Barth CA: Metabolic consequences of a high dietary-protein intake in adulthood: assessment of the available evidence. J Nutr 2000, 130(4):886-889.
Brenner BM, Meyer TW, Hostetter TH: Dietary protein intake and the progressive nature of kidney disease: the role of hemodynamically mediated glomerular injury in the patho- genesis of progressive glomerular sclerosis in aging, renal ablation, and intrinsic renal disease. N Engl J Med 1982, 307(11):652-659.
Calderon JL, Zadshir A, Norris K: A survey of kidney disease and risk-factor information on the World Wide Web. Med Gen Med 2004, 6(4):3.
Lindheimer MD, Katz AI: Physiology and Pathophysiology. In Renal physiology and disease in pregnancy 2nd edition. Edited by: Seldin DW, Giebisch G. New York , Raven Press ; 1992:3371–3431.
Food and Nutrition Board, Institute of Medicine: Macronutrient and Healthful Diets. In Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids (Macronutrients) Washington, D.C., The National Academies Press; 2002:609-696.
St. Jeor ST, Howard BV, Prewitt E et al. Dietary protein and weight reduction: A statement for health care professionals from the Nutrition Committee of the Council on Nutrition, Physical Activity, and Metabolism of the American Heart Association. Circulation 2001;104:1869-1874.
Street C. High-protein intake – Is it safe? In: Antonio J, Stout JR, eds. Sports Supplements. Philadelphia: Lippincott Williams & Wilkins, 2001, pp. 311-312.
Walser M. Effects of protein intake on renal function and on the development of renal disease. In: The Role of Protein and Amino Acids in Sustaining and Enhancing Performance. Committee on Military Nutrition Research, Institute of Medicine. Washington, DC: National Academies Press, 1999, pp. 137-154.
Poortmans JR, Dellalieux O. Do regular high-protein diets have potential health risks on kidney function in athletes? Int J Sports Nutr 2000;10:28-38.
Lentine K, Wrone EM. New insights into protein intake and progression of renal disease. Curr Opin Nephrol Hypertens 2004;13:333-336.
Campbell A. Tackling “diabesity” head-on. Joslin Diabetes Center’s new nutrition guideline. Diabetes Self Manag 2005;22:40, 42–4.
H Frank, J Graf, U Amann-Gassner, R Bratke, H Daniel, U Heemann, and H Hauner. Effect of short-term high-protein compared with normal-protein diets on renal hemodynamics and associated variables in healthy young men Am J Clin Nutr 2009;90:1509–16.
Lew SW, Bosch JP. Effect of diet on creatinine clearance and excretion in young and elderly healthy subjects and in patients with renal disease. J Am Soc Nephrol 1991;2:856–65.
Brandle E, Sieberth HG, Hautmann RE. Effect of chronic dietary protein intake on the renal function in healthy subjects. Eur J Clin Nutr 1996;50: 734–40.
Wiegmann TB, Zlomke AM, MacDougall ML, Kipp DE. Controlled changes in chronic dietary protein intake do not change glomerular filtration rate. Am J Kidney Dis 1990;15:147–54.
Bosch JP, Lew S, Glabman S, Lauer A. Renal hemodynamic changes in humans: response to protein loading in normal and diseased kidneys. Am J Med 1986;81:809–15.
Solerte SB, Rondanelli M, Giacchero R, et al. Serum glucagon concentration and hyperinsulinaemia influence renal haemodynamics and urinary protein loss in normotensive patients with central obesity. Int J Obes Relat Metab Disord 1999;23:997–1003.
Barba G, Cappuccio FP, Russo L, Stinga F, Iacone R, Strazzullo P. Renal function and blood pressure response to dietary salt restriction in normotensive men. Hypertension 1996;27:1160–4.
Ikizler TA. Nutrition support and management of renal disorders. In: Bronner, F. ed. Nutritional Aspects and Clinical Management of Chronic Disorders and Diseases. Boca Raton, FL: CRC Press, 2003, pp. 156-175.
Klahr S, Levey AS, Beck GJ et al. The effects of dietary protein restriction and blood-pressure control on the progression of chronic renal failure. N Engl J Med 1994;330:877-884.
American Diabetic Association. Evidence-based nutrition principles and recommendations for the treatment and prevention of diabetes and related complications. Diabetes Care 2002;25:S50-S60.
Gannon MC, Nuttall FQ, Saeed A et al. An increase in dietary protein improves the blood glucose response in persons with type 2 diabetes. Am J Clin Nutr 2003;78:734-41
Cooper C, Atkinson EJ, Hensrud DD et al. Dietary protein intake and bone mass in women. Calcif Tissue Int 1996;58:320-325.
Geinoz G, Rapin CH, Rizzoli R et al. Relationship between bone mineral density and dietary intakes in the elderly. Osteoporos Int 1993;3:242-8. 38. Michaelsson K, Holmberg L, Mallmin H. Diet, bone mass, and osteocalcin: a cross-sectional study. Calcif Tissue Int)1995;57:86-93.
Kerstetter JE, O ́Brien KO, Insogna KL. Dietary protein affects intestinal calcium absorption. Am J Clin Nutr 1998;68:859-865.
Kerstetter JE, Svastislee C, Caseria D et al. A threshold for low-protein-diet-induced elevations in parathyroid hormone. Am J Clin Nutr 2000;72:168-173.
Giannini S, Nobile M, Sartori L et al. Acute effects of moderate dietary protein restriction in patients with idiopathic hypercalciuria and calcium nephrolithiasis. Am J Clin Nutr 1999;69:267-271.
Schurch MA, Rizzoli R, Slosman D et al. Protein supplements increase serum insulin-like growth factor-I levels and attenuate proximal femur bone loss in patients with recent hip fracture: A randomized, double-blind, placebo-controlled trial. Annals Internal Med 1998;128:801-809.
Avenell A, Handoll H. Nutritional supplementation for hip fracture aftercare in the elderly. Cochrane Database Syst Rev 2004;1:CD001880.
Ginty F. Dietary protein and bone health. Proc Nutr Soc 2003;62:867-76.
Dawson-Hughes B, Harris SS, Rasmussen H et al. Effect of dietary protein supplements on calcium excretion in healthy older men and women. J Clin Endocrinol Metab 2004;89:1169-73
Obarzaneck E, Velletri PA, Cutler JA. Dietary protein and blood pressure. JAMA 1996;275:1598-1603.
Reed D, McGee D, Yano K, Hankin J. Diet, blood pressure, and multicollinearity. Hypertension 1985;7:405-410
Zhou B, Wu X, Tao SQ. Dietary patterns in 10 groups and the relationship with blood pressure. Collaborative Study Group for Cardiovascular Diseases and their Risk Factors. Chin Med J 1989;102:257-261
Stamler JS, Caggiuala A, Grandist GA. Relationship of dietary variables to blood pressure (BP) findings of the Multiple Risk Factors Intervention Study (MRFIT). Circulation 1992;85:867, Abstract 23.
Kuchel O. Differential catecholamine responses to protein intake in healthy and hypertensive subjects. Am J Physiol 1998;R1164-R1173.
Hu FB, Stampfer MJ, Manson JA et al. Dietary protein and risk of ischemic heart disease in women. Am J Clin Nutr 1999;70:221-227.
Navder KP, Lieber CS. Nutritional support in chronic disease of the gastrointestinal tract and the liver. In: Bronner, F. ed. Nutritional Aspects and Clinical Management of Chronic Disorders and Diseases. Boca Raton, FL: CRC Press, 2003, pp. 45-68.
Volek JS, Sharman MJ, Love DM et al. Body composition and hormonal responses to a carbohydrate-restricted diet.Metabolism 2002;51:864-870
Srivastava N, Singh N, Joshi YK. Nutrition in management of hepatic encephalopathy. Trop Gastoenterol 2003;24:59-62
Feinman RD, Fine EJ. Thermodynamics and metabolic advantage of weight loss diets. Metab Synd Relat Disord 2003;1:209-219.

 Argentina
Argentina
 Österreich
Österreich Australia
Australia Brasil
Brasil Canada
Canada Canada (Français)
Canada (Français) Schweiz
Schweiz Suisse (Français)
Suisse (Français) Svizzera (Italiano)
Svizzera (Italiano) Deutschland
Deutschland España
España France
France Great Britain
Great Britain Portugal
Portugal Usa
Usa Usa (Español)
Usa (Español)