
Hepatic Steatosis, alias Fatty Liver, is a liver disease with different etiologies and it can be mainly distinguished in alcoholic and non-alcoholic. In this second case, the root cause is given by excessive fat deposit (in the form of triglycerides) within the liver. It becomes detectable via ultrasound when the triglyceride deposit exceeds approximately 30% of the weight of the organ.
There is evidence in literature that in the presence of (radiologically) ascertained steatosis the relationship among blood transaminases may be suggestive of the (alcoholic or non-alcoholic) pathogenesis. In particular, an AST/ALT ratio greater than 2 expresses a steatosis more likely of alcoholic origin, a ratio of less than 1 is more suggestive of a steatosis of non-alcoholic origin.
A hypothesis that is often indicated by nutrition experts against diets causing quick weight loss is that if the weight lost is superior to 5 kg a month, they cause a confluence of fatty acids, mobilized from adipose tissue, higher than the management capability of the organ. Excess acid fats will therefore be deposited in the liver, and lacking the means of being disposed, they will induce the appearance, or worsening, of steatosis.
For this purpose, we examined customers who had been activated in the 2015 course following the Platinum program. Out of all these customers, 1,067 provided the full values of AST and ALT at the beginning of the program and after 60 days.
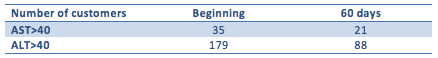
The excessive value of one of these two parameters is a criterion for exclusion from the program, reason why you will not encounter very high values in the initial tests. In particular, the total number of customers was 35 with ALT over 40 and 179 with AST over 40.
After 60 days from the beginning of the Program 21 customers showed AST levels over 40 and 88 customers ALT levels over 40.

As for the relationship AST/ALT, at the beginning of the Program, there were 718 customers with a ratio below 1 (therefore with possible non-alcoholic steatosis, average 0.72), after 60 days the number of individuals with ratio below 1 was 596 (with an average of 0.75).
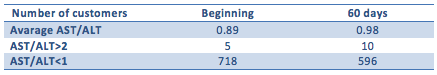
Considering instead the hypothesis that rapid weight loss (more than 5 kg per month) induces to steatosis, we analyzed the performance of the parameters available only in the population of clients who lost more than 10 kg in the first 60 days of the Program, that is a total of 640 individuals, with an average loss of 13.74 kg.
The results of blood test parameters considered in this analysis are summarized in the following table.
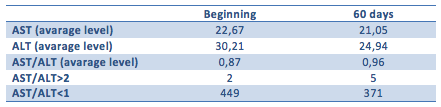
In conclusion therefore, although no initial radiological diagnosis of steatosis was available and being unable to assess via ultrasound the situation of the liver in the two observation points, it can be concluded that the transaminases (i.e. the indicators of liver damage), in absolute value, averagely improved over time.
Moreover, the number of clients with ratio of NAFLD transaminases is reduced after 60 days’ Program compared to the beginning, and this also works for those losing more than 10 kg in the first two months of the Program.
Further evaluations are necessary to confirm the data and it would be interesting to present a group of customers to ultrasound evaluation at the beginning of the Program, at 60 and again at 150 days into the program to validate these results that, if confirmed, would be an important and indisputable indicator of the improvement of our customers’ state of health.

 Argentina
Argentina
 Österreich
Österreich Australia
Australia Brasil
Brasil Canada
Canada Canada (Français)
Canada (Français) Schweiz
Schweiz Suisse (Français)
Suisse (Français) Svizzera (Italiano)
Svizzera (Italiano) Deutschland
Deutschland España
España France
France Great Britain
Great Britain Portugal
Portugal Usa
Usa Usa (Español)
Usa (Español)